Trending



 Crocs launches new Height collectionEvan-Lee Courie
Crocs launches new Height collectionEvan-Lee Courie New app to help Western Cape social workersMarecia Damons
New app to help Western Cape social workersMarecia Damons
#Designindaba2018: SA's crowd-sourced solution for a global problem

One of the triggers for the idea was bumping into a patient after he worked in a rural hospital in the Eastern Cape, where he had written a referral to see a specialist in Umtata as he did not know how to treat him due to lack of expertise at that stage. Seven years later, he learned that the patient had lost vision in one eye, as he had never got to the specialist. Mapham knew that he had had access to the information at the time, the medication had been actually available in the clinic and he would have been able to save an eye.
To give you a better perspective, in South Africa, the private health care system has about 1 doctor and 1 specialist for 1,500 people, and in the public system, there is 1 doctor for 4,500 people and only 1 specialist for 18,000 people. Mapham recalls when working in a clinic in the Eastern Cape even trying to get a telephone installed in a rural area proved trying as they need a street address in order to install a landline. Long story short, he ultimately gave the address - No 1, Dirt Road, Elliotdale – a town 45 minutes away, and eventually someone came out. Even so, they could only manage to get a radio link instead of a landline, but it was clear that something had to change… and the advent of mobile became the enabler.
How it works
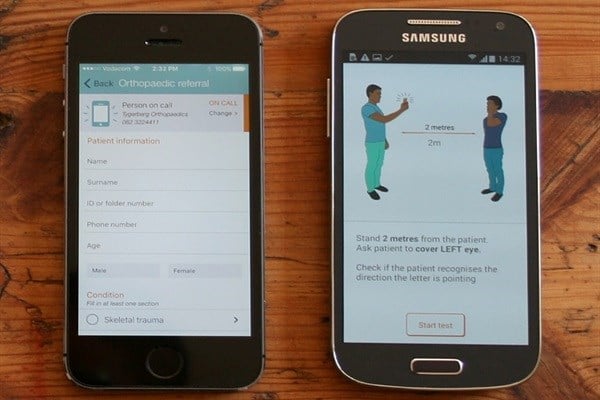
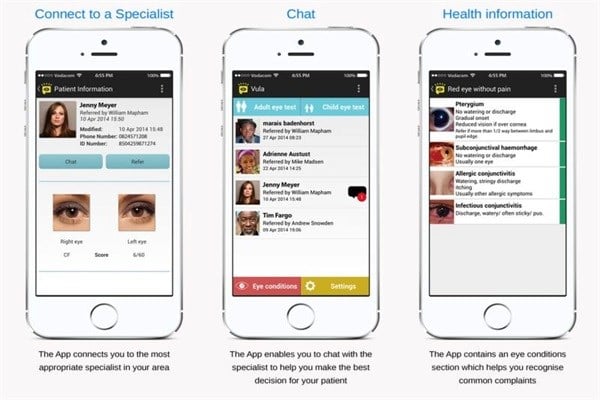
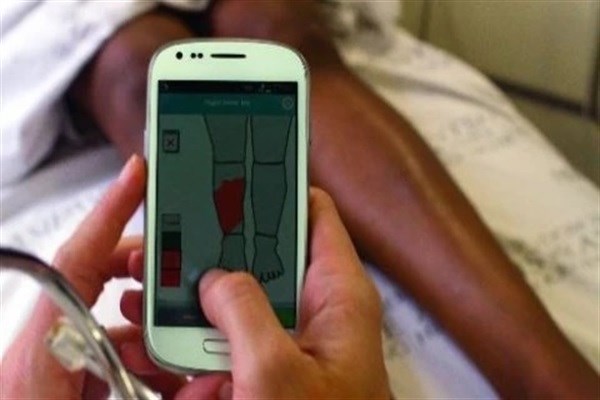
Essentially the Vula app helps ensure patients get the right care when they need it. Its a secure medical chat and referral application that’s designed to help healthcare workers to, quickly and efficiently, make and receive referrals with 4,000 medical specialists in 15 specially fields – ophthalmology, cardiology, orthopaedic, burns, HIV, dermatology, ENT, paediatrics, oncology, gynaecology, family medicine, general surgery, internal medicine and neurosurgery at present.
The chat functionality helps the health workers and specialists who are time sensitive work in an asynchronistic way and current response times are under 15 minutes – weirdly enough they find the least tech people respond the fastest!
Not only has it been a great success in treating patients, but also the educational aspect of self-training is high. From a doctor at Baragwanath to a sister in Vredendal who trained herself case by case remotely and managed to raise money from Japan to open her own clinic. Plus the amount of crowd-sourced data captured – they currently hold over 80,000 photographs – is so significant it’s proving to be an invaluable asset not only to health workers and specialists but health organisations, too.
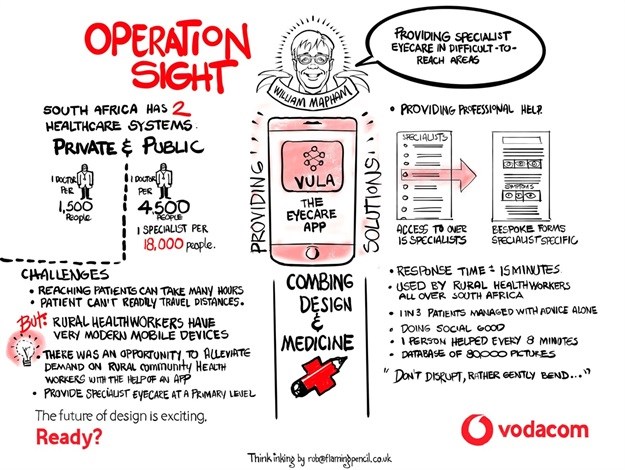
When asked what happens with the data, Mapham said, “The heads of departments can actually monitor what is going on in real-time, which enables clinical governance, which is how they actually manage peoples actual care. People have never seen this before because you can’t monitor everyone’s landline phone call, but we are monitoring all the advice going out and it's being used in teaching cases.”
To Africa and beyond
So what about expansion plans? His answer was, “we get asked all the time, not just from African countries, but the likes of Cambodia, New Zealand and others and the challenge there is, ‘Who is the health worker?’ the biggest problem is validation. In SA we have access to medical records, so we know exactly who is a health worker, and only health workers are allowed onto Vula.” In fact, he joked at the beginning of his talk he is probably the only person who doesn’t encourage the general public to download the app.
He carries on, “The biggest problem and actually it’s a design problem, but how do we role out to countries that don’t have that? In Namibia for example, all the health records are in a room – you can’t send someone to check every time someone tries to register, so the design team is looking at ways to solve that and once that’s done we can say ‘yes’ to people overseas, but until now we have actually resisted.”
As a start-up, Vula has always battled with funding, and the development of the app so far has been largely reliant on money from prizes for innovation and entrepreneurship.
Initial funding came via a flash grant (R50,000) from the Shuttleworth Foundation and donation of time to design and create a prototype by Debré Barrett and her team at Flow Interactive (now part of Deloitte Digital), which helped Mapham win the SAB Foundation Social Innovation Award in 2013. That prize money ensured the launch of the Android and iOS app in 2014 and since launch, they have won Most Innovative App at the MTN App of The Year in 2015, first prize at the 2016 Clearly Vision Prize awards and more recently a Platinum Award at the Impumelelo Social Innovations Awards.
The company was almost “flatlining” (his words) in 2016, but after Barrett joined on a permanent basis, they started to see some exponential growth and a huge increase in uptake and by default the value of the app became a much more viable option for investors and interested parties – which Will Green now handles from a commercial point of view.
They have developed a tiered system for the likes of the banking, insurance and medical industries to gain access over the 4,000 time-pressed medical practitioners. Not only will it facilitate corporate involvement, but the partnerships will enable keeping the app free.
And the future?
The dream is videos – like a Suzelle of how to do medical procedures.Mapham finished his talk with a video, which was captured after performing cataract surgeries on several patients in De Aar recently. One lady had not been able to see for 9 years and had to be helped all the time. Then through one surgery, suddenly she could see – her thankful tears made us all cry, too and the standing ovation that followed reiterated his opening words: “Some people say nothing good comes out of the Eastern Cape – Mandela came from there…”
To find out more, click here.