Top stories



Marketing & MediaHow Spar is using localised marketing to redefine the urban retail experience
Karabo Ledwaba 1 day



More news





ESG & Sustainability
How South Africa’s conservation efforts can thrive with Indian partnership









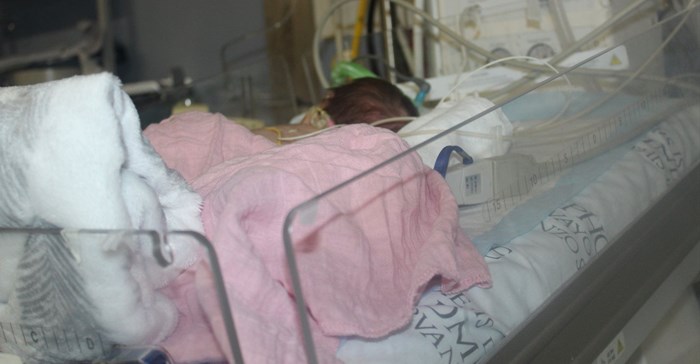
21-year-old Kiara Jackson, otherwise healthy, had been followed up at the Fetal Medicine Unit (FMU) of TBH since 21 weeks gestation because her fetus had a tumor in the mouth, likely a teratoma (usually benign).
Kiara was counselled about the findings and implications of the abnormality. She was told that likely the tumor would grow in size and this could cause complications. It could obstruct the airway or esophagus of the fetus, resulting in polyhydramnios (too much fluid surrounding the fetus in the womb) which could lead to early labour or early breaking of the waters.
Furthermore, the fetus could develop heart failure over time due to the high blood flow feeding the tumour. Kiara was informed that the delivery of the baby would be complicated with risks for her and baby, and that her baby would require an EXIT procedure. Additionally, the baby would also need surgery after birth that could result in damage to her vocal cords, nerves or vessels. There was also a small risk of malignancy of the tumour.
Kiara chose to continue with the pregnancy despite all the risks involved and was regularly seen in the FMU. On the last review at 35 weeks, the tumour measured 114 by 16 by 87mm, forcing the fetal mouth wide open.
“An extensive team of medical subspecialists at TBH performed a successful EXIT procedure on 10 December, 2021 by only half-delivering a baby to create a gap of 30 minutes for treatment while continuing oxygen supply by means of the placenta. In that period, a team of doctors used multiple methods to establish an airway for the baby because she couldn’t breathe spontaneously due to the presence of the very large tumour in her throat, which protruded from her mouth.
"We believe this to be the first of its kind in South Africa and are very proud of the team spirit of all involved roleplayers (six different teams with their own staff and equipment!) that made it possible to carry out this procedure with less than 24 hours' notice - as the mother showed signs of impending labour before the planned surgery date,” explains Prof Lut Geerts.
The purpose of the procedure was to establish an airway for the baby while it was still receiving oxygen from the placenta because it was only half-delivered during caesarean section with the placenta still attached to the uterine wall. This is necessary in cases where spontaneous breathing at birth is feared not to be possible due to growths of the fetal neck or in the mouth. for example.
The planning of the procedure involved a multidisciplinary meeting involving the main team members, which was held on 6 December when the patient was 34 weeks and 5 days pregnant. She had an MRI of the fetus so all colleagues could visualise the anatomy.
The team members were Prof L Geerts (head of Fetal Medicine Unit); Prof P Goussard (paediatric pulmonologist); Dr C de Vos (paediatric surgeon); Dr A Breedt (qnaesthesiologist for baby); Dr JL Burke (anaesthesiologist for mother); Dr M Merven (ear, nose and throat specialist); Dr HA Swart (obstetrician and gynaecologist); and Dr L van Wyk (neonatologist).
The decision was a planned delivery by means of EXIT procedure on 15 December at 36 weeks’ gestation. The patient was reviewed three days later at the FMU and found to be at high risk of going into early labour (short cervix and high volumes of amniotic fluid). The reviewed decision was to deliver the baby the next morning at 35 weeks and two days gestation. High level arrangements were made at short notice to get everything in place.
The EXIT procedure took place on 10 December at Tygerberg Hospital.
Dr A Breedt provided general anaesthesia for Kiara (specific goals were deep anaesthesia and a completely relaxed uterus during the EXIT procedure, with good contraction of the uterus after delivery of the baby). Prof Geerts performed an amniodrainage (1 litre of fluid around the baby was drained by means of a needle into the womb before the operation started, to decrease the amount of fluid that might gush out during the surgery and result in the baby’s cord or body being pushed out of the uterus or the placenta detaching from the uterine wall).
A caesarean section was performed by Drs HA Swart and C von Drünick (assistant). Srs J January, S Smith, staff nurse A Moses and nurse M Gantsho all played vital roles in theater.
Only the baby girl’s head and neck and her right arm (for monitoring purposes) were gently delivered via the incision. Dr C Apollos performed an amnio-infusion during the surgery (warm fluid running into the uterus to avoid all the fluid draining out and the placenta detaching from the uterine wall due to the shrinking uterine volume).
While the rest of the baby’s body was still in the uterus, attached to the placenta and thus receiving oxygen from the mother (as the baby could not breathe on her own due to the teratoma obstructing her whole mouth and nose), the goal was to secure an airway for the baby to be able to be ventilated by means of a tube.
Dr J Burke gave anaesthetic agents into the baby's arm to keep her calm and avoid her feeling pain. Dr C de Vos took responsibility to handle the tumour, to keep it from being injured. and to advise on options of establishing an airway.
Prof P Goussard and Dr M Merven took responsibility to establish the baby’s airway. They did this by attempting different routes (via baby’s nose and mouth) and with different instruments including videolaryngoscopy (trans-oral) and flexible bronchoscopy.
Establishing an airway was very challenging due to the size and position of the tumour in the baby’s mouth. After 30 minutes an airway was established via a tube through the baby’s mouth.
The baby was then fully delivered and further managed in the baby crib in theater. There, the oral tube was exchanged for a nasal tube under direct vision (as this is more stable with less change of accidentally slipping out).
The baby was then taken to the neonatal intensive care unit (ICU) in a stable condition (under the care of Dr L Van Wyk). Most of the oral tumour could be removed by the paediatric surgery team five days later, on 15 December.
The baby girl has been named Ivoree Jane and is currently stable, still in the neonatal ICU for supportive care. While Ivoree Jane can breathe well, there are still problems with her feeding and inability to close her mouth properly, which are being addressed.
Kiara’s surgery was completed as soon as her baby was delivered. She was given medication to contract the uterus firmly in order to prevent bleeding. Afterwards, she was observed in a high care setting for 24 hours due to high risk of bleeding from her uterus.
Kiara was discharged two days later with no complications from the surgery and visits Ivoree Jane daily in the NICU.