Trending




 Sabre EMEA 2024 Awards: Razor PR, Retroviral top SA agenciesDanette Breitenbach
Sabre EMEA 2024 Awards: Razor PR, Retroviral top SA agenciesDanette Breitenbach
Elections 2024
New strategy to reduce the number of mothers and babies at risk
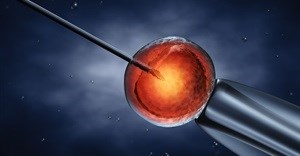
More than a quarter of in vitro fertilization (IVF) conceptions result in multiple births, which are far more likely to result in premature or other forms of problematic births. According to a new report* by independent market analyst Datamonitor, almost 40,000 British women will have infertility treatment in 2007, however, HFEA's new strategy will greatly reduce the number of mothers and babies at risk.
The potential negative consequences of multiple births
Many assisted pregnancies have led to multiple births following excessive follicular stimulation in ovulation induction cycles and multiple embryo transfers, which are practiced in order to increase the chances of success. European and US registries of assisted reproduction indicate that 25% of IVF and intracytoplasmic sperm injection (ICSI) cycles result in twins and another 3-5% result in higher order multiple pregnancies (HOMP)(1). In addition to the potentially fatal ovarian hyperstimulation syndrome (OHSS), multiple pregnancies have been associated with a statistical increase in maternal risk for obstetric complications, congenital malformations and long-term neurological conditions, and lower gestational age and birth weight.
According to Datamonitor women's health analyst Anna Nesbitt, the wider implications of multiple births must also be considered. “The healthcare costs of neonatal and delivery services are increased for multiple pregnancies and the pressure of raising more than one child can generate familial complications of a psychological, social and financial nature which are further exacerbated by disability,” she says.
Calls for tighter regulation
These concerns over mother and baby safety have seen a move towards milder stimulation protocols in recent years and Datamonitor predicts that this trend is set to continue. Shorter stimulation protocols involve a gonadotropin-releasing hormone (GnRH) antagonist co-treatment with a low dose gonadotropin and single rather than multiple embryo transfer. The HFEA has announced that they expect multiple birth rates to fall so that they account for just 10% of all IVF pregnancies and have called on professional bodies to develop an all-encompassing, national strategy to ensure this prediction is met.
Work on these guidelines is due to begin immediately and with the first discussion scheduled in February 2008, change for the UK infertility market is imminent.
IVF in the UK
There are around 80 clinics in the UK that offer some form of infertility treatment. While 30% are NHS practices, private patients can also be treated there. The market is boosted by partial reimbursement of treatment, making assisted reproductive technology (ART) accessible to more than just the very wealthy. Datamonitor estimates that in 2007, 38,000 British women were willing and able to have infertility treatment and based on this, forecasts the UK infertility drug market to be worth around $95million. Additionally, Datamonitor forecasts the seven major markets** combined to be worth $3.5 billion in 2007, the majority of which is generated by three large pharmaceutical companies: Ferring, Merck Serono and Organon.
Winners and losers
A reduction in the number of multiple births will have several impacts on current treatment cycles. The transfer of a single embryo is likely to be enforced and the use of mild stimulation protocols is likely to become more widespread. Market players will feel the result of a reduction in the administration of gonadotrophins as a reduction in sales volume. However, Nesbitt sees an upside in the situation. “The shorter stimulation protocol and the transfer of a single embryo may allow more IVF cycles to be conducted within the same period of time as conventional treatment. More cycles will require more drugs and with careful management of pricing and reimbursement strategies, revenue may even increase,” she says.
A key consideration in this debate is the infertile couples themselves. For some, the desire to conceive may be so great that they are willing to risk the complications of a multiple pregnancy. Others will prefer the safer, faster and less expensive mild stimulation protocol, and the ethics of removing a patient's choice must be considered.
In Belgium, because of savings made in reducing multiple births, a reimbursement system has been funded which allows couples six IVF/ICSI cycles in a lifetime. Results the first year after implementation show an increase in the total number of treatment cycles is advantageous for the industry and patients alike.
Other market forces
As infertility treatment becomes more accessible, the improving success rates of IVF treatment across key markets will continue to boost the number of cycles initiated. As a European expert told Datamonitor: “As IVF becomes a more standard procedure, the more confident we become that these children are doing well, the more it will be liberally employed”.
Additionally, a range of embryological techniques, such as in vitro maturation, cryopreservation and microarrays are currently being refined and will rapidly expand the treatable patient population as all women with the intention of preserving and protecting embryos will be eligible for treatment, not just those that are infertile, Nesbitt says. “The trend towards later parenthood will also increase the number of women eligible for infertility treatment.
“Given these factors, growth of the infertility market looks certain. With careful monitoring of the regulations called for by the HFEA, the trend towards single births has the potential to benefit both the patient and infertility industry while delivering the ultimate goal, a much desired, healthy child,” she says.